Can you screen for Lung cancer ?
Yes we can screen for Lung cancer with Low Dose Ct scans of the Chest
Who Should be screened for lung cancer ?
Evidence suggests this is more useful for those individuals above 55 years of age and for those who are smokers or have been smokers
What are the benefits of Lung Cancer Screening
Early Detection: Screening can catch lung cancer at an early stage when treatment is more likely to be effective. This can increase the chances of survival.
Targeted Screening: Focusing on people at higher risk makes lung cancer screening more effective in saving lives.
Risks /Pitfalls of Lung Cancer Screening
Radiation Exposure: Each CT scan involves a small amount of radiation. Repeated exposure over time could potentially cause harm to the lungs.
False Positives: Sometimes, the scan might detect something that appears to be cancer but isn’t. This can lead to unnecessary further tests which can cause anxiety .
False Negatives: Rarely the Screening test may miss a cancer that is present, giving a false sense of security.
Overdiagnosis: Screening may detect lung cancers that would never have caused any problems during a person’s lifetime. This could lead to unnecessary treatments, including surgery, radiation, or chemotherapy, which have their own risks and side effects.
How do I decide if Lung Cancer screening is for me ?
Knowing the benefits and risks of lung cancer screening is vital in making the decision that’s appropriate for you.
● ABOUT DR ANAND SINGH
About Dr Anand Singh
Dr Anand Singh is a highly experienced Consultant Respiratory Physician with over a decade of experience in the field.
Dr Singh is a well known Chest Consultant and Sleep Consultant who provides personalised treatment plan.
Dr Anand Singh is a consultant Respiratory Physician at West Hertfordshire Teaching Hospitals NHS Trust
(Watford General and Hemel Hempstead Hospital where he leads the Sleep and Non-Invasive ventilation Service
and Respiratory High Dependency unit. He undertakes sub-speciality clinics in Interstitial Lung diseases
and Sleep Apnoea as well as conducting general respiratory medicine clinics.
Professional Memberships


Recommended by patients
What do you mean by Chronic Respiratory Failure?
Chronic respiratory failure is the inability to carry out the fundamental functions of respiration. The lungs function to deliver oxygen to the blood while eliminating carbon dioxide from the blood. It is a condition that usually occurs from narrow or damaged airways that develop gradually over time with a progressive underlying process that requires long-term treatment.
Causes of Chronic Respiratory Failure
Conditions /diseases that affect your breathing can cause chronic respiratory failure and may include:
- Pneumonia
- Interstitial Lung disease
- Chronic obstructive pulmonary disease (COPD)
- Smoking
- Drug or alcohol abuse
- Chest trauma
- Cystic fibrosis
- Muscular dystrophy
- Motor Neuron Disease
- Stroke
- Spinal cord complications
Symptoms Associated with Chronic Respiratory Failure
Symptoms of chronic respiratory failure may include:
- Breathlessness
- Coughing
- Wheezing
- Fast breathing
- Headache
- Anxiety
- Fatigue
- Confusion
- Bluish colouration of the lips, fingernails, or skin
- Abnormal heart rhythm
How is Chronic Respiratory Failure Diagnosed
This is based on:
- Medical history and symptoms
- Your physical examination.
- Pulse oximetry test, which is conducted to evaluate how well oxygen is being delivered to various parts of the body. Normal oxygen saturation will range above 94 , and anything under 90 per cent would indicate an abnormally low level of oxygen.
- Arterial blood gas test, which is conducted to measure the amount of oxygen and carbon dioxide in your blood and any abnormal level would indicate chronic respiratory failure.
- Imaging tests, such as chest x-ray or CT scan, to get a better view of your lungs, which may reveal potential causes of chronic respiratory failure.
- Bronchoscopy
How is Chronic Respiratory Failure Treated?
The aim of the treatment is to get oxygen to your lungs and other organs and remove carbon dioxide from your body. The common treatment options used to achieve these may include:
- Ventilator: A breathing machine that pumps oxygen into your lungs and removes carbon dioxide from your lungs through a tube placed into your nose or mouth down into your windpipe.
- Oxygen therapy: This therapy raises oxygen levels by increasing the amount of oxygen you inhale by delivering oxygen from a concentrator / cylinder
- Tracheostomy: A surgical procedure where a hole is made through the front of your neck and into your windpipe for a breathing tube to pass through to help you breathe.
- Other breathing treatments: Non invasive positive pressure ventilation (NIV) where air pressure is used to keep your airways open .Noninvasive ventilation includes Bipap devices . Cpap devices can be used as well
- Treatment of the underlying cause
● ABOUT DR ANAND SINGH
About Dr Anand Singh
Dr Anand Singh is a highly experienced Consultant Respiratory Physician with over a decade of experience in the field.
Dr Singh is a well known Chest Consultant and Sleep Consultant who provides personalised treatment plan.
Dr Anand Singh is a consultant Respiratory Physician at West Hertfordshire Teaching Hospitals NHS Trust
(Watford General and Hemel Hempstead Hospital where he leads the Sleep and Non-Invasive ventilation Service
and Respiratory High Dependency unit. He undertakes sub-speciality clinics in Interstitial Lung diseases
and Sleep Apnoea as well as conducting general respiratory medicine clinics.
Professional Memberships


Recommended by patients
A chronic cough is defined as a cough which lasts three weeks or more and requires medical evaluation. While chronic cough may often be due to non-serious and treatable causes, it is crucial to determine the underlying cause to provide appropriate treatment.
Common Causes of Chronic Cough:
– Asthma
– Interstitial Lung disease
– Rhinitis and sinusitis
– Postnasal drip
– Acid reflux
– Chronic bronchitis
– Upper-Airway Cough Syndrome (UACS)
– Infections
– Bronchiectasis
Approach to Diagnosing Chronic Cough
The first step involves a detailed medical history and physical examination to identify possible causes.
Investigations :
Depending on initial findings, tests such as blood tests, allergy screens, CT scans, and lung function tests may be necessary to identify the exact cause.
Management:
Most cases of chronic cough can be diagnosed and treated effectively based on these assessments . In some instances, no cause can be identified.
● ABOUT DR ANAND SINGH
About Dr Anand Singh
Dr Anand Singh is a highly experienced Consultant Respiratory Physician with over a decade of experience in the field.
Dr Singh is a well known Chest Consultant and Sleep Consultant who provides personalised treatment plan.
Dr Anand Singh is a consultant Respiratory Physician at West Hertfordshire Teaching Hospitals NHS Trust
(Watford General and Hemel Hempstead Hospital where he leads the Sleep and Non-Invasive ventilation Service
and Respiratory High Dependency unit. He undertakes sub-speciality clinics in Interstitial Lung diseases
and Sleep Apnoea as well as conducting general respiratory medicine clinics.
Professional Memberships


Recommended by patients
What is Bronchiectasis?
Bronchiectasis is a chronic / long term condition where the airways (bronchi) of your lungs are inflamed, infected, and permanently damaged.
Why Causes Bronchiectasis Happen and How Does it Affect You?
If your lungs are injured, there will be inflammation and/or infection present in your bronchi. This leads to the accumulation of mucus and thickening of the walls of your bronchi. The condition finally results in a cycle of bacterial infection, a pool of mucus in your lungs, blockages in your bronchi, and gradual decline in your lung function over time. In the end, you will have difficulty with breathing.
What are the Risk Factors and Causes of Bronchiectasis?
Any sort of lung injury can lead to bronchiectasis and it can sometimes affect your whole body. You may also develop bronchiectasis if you have any of the following conditions:
- A whooping cough and tuberculosis (forms of lung infections)
- Humoral immunodeficiency (blood with low levels of infection-fighting proteins or abnormally functioning immune system)
- Inflammatory bowel disease (Crohn’s disease and ulcerative colitis)
- Rheumatologic diseases (rheumatoid arthritis and Sjögren’s disease)
- Alpha1-antitrypsin deficiency (COPD caused by a genetic factor)
- Chronic obstructive pulmonary disease or COPD
- Infection with HIV or autoimmune diseases
- Allergic bronchopulmonary aspergillosis (an allergic lung inflammation)
Symptoms of Bronchiectasis
Symptoms of typical bronchiectasis may take several months or even years to develop and manifest. Therefore, you should see your doctor for diagnosis and treatment if you:
- Notice frequent respiratory infections
- Have a chronic cough and discharge of blood or mucus mixed with blood
- Are coughing up a large amount of thick yellow or green mucus regularly
- Produce abnormal or wheezing or whistling sound while breathing
- Have chest pain and shortness of breath
- Suffer from fatigue and unintended weight loss
- Notice change in the structure of your fingernails or toenails
How can Bronchiectasis be Diagnosed?
Your doctor will first listen to your lungs and check for airway blockage or any abnormal sounds while you breathe. Several tests may be ordered to diagnose the condition, including:
- Complete blood test for the possibility of infection and anaemia
- Sputum test for the presence of viruses or bacteria or fungi in your mucus
- Chest X-ray or CT scan to have a look at your lung structure
- Pulmonary test to find out how normally your lungs are functioning
- Purified protein derivative (PPD) skin test or QuantiFERON blood test to check for tuberculosis
- Sweat test to screen for Cystic Fibrosis (CF), a type of bronchiectasis
What are the Possible Treatments of Bronchiectasis?
Bronchiectasis cannot be cured. However, it can be managed and kept under control by the following methods:
- Antibiotic therapy
- Mucus thinning therapy
- Oxygen therapy
- Chest physiotherapy
- Pulmonary rehabilitation
- Vaccination
- Bronchodilators remedy
- Expectorants remedy
- Breathing exercises
With early diagnosis and appropriate treatment, you may be able to lead a normal life.
Prevention of Bronchiectasis
In most cases, the exact cause of bronchiectasis cannot be found. Apart from vaccination, avoiding smoking or polluted air or toxic fumes or dust seem to be the best way to prevent bronchiectasis and save your lungs.
● ABOUT DR ANAND SINGH
About Dr Anand Singh
Dr Anand Singh is a highly experienced Consultant Respiratory Physician with over a decade of experience in the field.
Dr Singh is a well known Chest Consultant and Sleep Consultant who provides personalised treatment plan.
Dr Anand Singh is a consultant Respiratory Physician at West Hertfordshire Teaching Hospitals NHS Trust
(Watford General and Hemel Hempstead Hospital where he leads the Sleep and Non-Invasive ventilation Service
and Respiratory High Dependency unit. He undertakes sub-speciality clinics in Interstitial Lung diseases
and Sleep Apnoea as well as conducting general respiratory medicine clinics.
Professional Memberships


Recommended by patients
What is a sleep study?
Sleep studies encompass many general tests and sleep problems. When focusing solely on respiratory issues, the tests that are usually used include:
- Respiratory polygraphy sleep test / Multi Channel Sleep study
- Recording oxygen levels overnight
- Polysomnography (PSG)
Sleep studies are often conducted in the evening as that’s when most patients go to sleep.
Depending on the monitoring equipment required for the test, many patients can do a test themselves at home; for example, sleep apnoea tests can be done in your own home.
To be certain that you require a test from the sleep centre, you’ll first need to contact us and book an initial appointment. During this appointment, the doctor will run a few tests and assess whether you have symptoms associated with sleep-disordered breathing (SDB):
- Waking from a full night of sleep , still feeling tired
- Daytime sleepiness
- Headaches in the morning
- Gasping, snorting, loud snoring, or choking during sleep
- A disturbed sleep
- Low oxygen levels
- High carbon dioxide levels
- Breathing that stops and starts while you sleep
If you’re not sure if you have these symptoms, but you think you may need a sleep test, record yourself at night so that you can listen back and assess whether you need to make an appointment with us.
In general, a sleep test not only offers you a diagnosis, but it also helps the doctor create an appropriate and personalised treatment plan for you.
Before
As mentioned previously, to gain access to a sleep study, you’ll first need to arrange an appointment with Dr Singh. The doctor will then ask a few questions and may run some tests to determine whether a sleep study is right for you .
For further information, the doctor will also discuss your symptoms, ask you to complete a sleep questionnaire, discuss how long you’ve been impacted, your medical history, and whether you take any medication (for example, sleeping tablets, anti-depressants, or prescribed painkillers).
If you’re given the go-ahead to start a sleep study, there are protocols all patients must follow before their test to not interfere with the results. For example:
- Avoid alcohol and caffeine
- Avoid napping prior to the test
You should be able to continue taking any regular medications – unless the doctor specifies otherwise.
During
A sleep study includes a range of tests. When a sleep specialist needs to monitor your respiratory system, you can expect them to recommend one of those three tests:
Multi-channel Sleep Study /Respiratory polygraphy sleep test
A respiratory polygraphy is a test that can diagnose different types of breathing difficulties and assess their severity.
This type of test is usually conducted at home. The equipment can be picked up from the hospital and will include a chest and abdomen band to measure movement, a small flow sensor in the nostrils, and an oxygen monitor on the finger; you’ll need to wear these during the test.
The equipment is used to diagnose sleep-disordered breathing (SDB), which can diagnose conditions such as obstructive sleep apnoea (OSA).
While you wear the equipment, it will record your:
- Breathing
- Oxygen levels
- Heart rate
- Snoring
- Sleep position and movement.
Overnight oximetry
When focusing on your respiratory system, sometimes a sleep consultant will run a recording of your oxygen levels overnight.
Most often, this test is used to diagnose a sleep condition or ensure the current treatment plan you’re on is effective.
This test may require an overnight stay; however, sometimes you’re able to pick it up and take it away with you. Before you fall asleep, you’ll put a small clip called a pulse oximeter on your finger (sometimes your earlobe), which will record your oxygen levels and heart rate overnight.
Patients with no underlying cardio-respiratory disease will have an oxygen level of between 95% – 98% at rest, however, if your oxygen level dips by 4% of that healthy range, then it could indicate that you’ve been holding your breath for at least 10 seconds. This disrupted sleep is concerning as it can be indicative of a larger problem or lead to other illnesses developing.
Polysomnography (PSG)
This tests is lest commonly done nowdays .
A PSG is a piece of equipment that you can collect from the sleep centre and take away to use at home (but you will need to return it to the clinic the next day), however, you might be required you to wear it for an overnight stay.
A neurological sleep study will be recommended if you are showing signs of having a neurological sleep disorder. During the test you will wear breathing bands around the chest and abdomen and small disposable discs on your head attached using sticky water-soluble paste. Additional electrodes will be applied on the shoulder area to record heart rate and on the calf muscles to record muscle activity.
The sensors will then monitor your sleep and send the data to the team. A PSG is designed to assess:
- Brain activity
- Eye movements
- Heart rhythm
- Breathing signals
- Oxygen levels
The data gained from a PSG can help the team rule out sleep disorders such as obstructive sleep apnoea, narcolepsy, sleep-related seizure disorders, chronic insomnia, and more.
It’s important that you do reach out to the sleep centre for a diagnosis because if you are living with an untreated disorder, then it can raise your risk of:
- heart disease
- high blood pressure
- stroke
- depression
After
As each test requires you to be asleep, we typically require a full night’s worth of data for the most accurate reading.
If you had the test done at home, you’ll need to return the equipment the next morning.
Regardless of the test that was performed on you, you’ll need to allow some time for the team to assess the data and review the information; this typically will take around a week.
Once your results are back in, you’ll be able to schedule a follow-up appointment. In this appointment, Dr Singh will go through the results with you. Based on these results and your symptoms, you’ll be given your diagnosis.
After the diagnosis, Dr Singh will work through a personalised treatment plan with you.
● ABOUT DR ANAND SINGH
About Dr Anand Singh
Dr Anand Singh is a highly experienced Consultant Respiratory Physician with over a decade of experience in the field.
Dr Singh is a well known Chest Consultant and Sleep Consultant who provides personalised treatment plan.
Dr Anand Singh is a consultant Respiratory Physician at West Hertfordshire Teaching Hospitals NHS Trust
(Watford General and Hemel Hempstead Hospital where he leads the Sleep and Non-Invasive ventilation Service
and Respiratory High Dependency unit. He undertakes sub-speciality clinics in Interstitial Lung diseases
and Sleep Apnoea as well as conducting general respiratory medicine clinics.
Professional Memberships


Recommended by patients
What is Asthma?
Asthma is an inflammatory disease of the airways to the lungs. It makes breathing difficult and can make some physical activities difficult or even impossible. Dr. Anand Singh is an asthma specialist at The Clementine Churchill Hospital in Harrow, and Syon Clinic in Brentford, West London, OSD Healthcare Hertfordshire with more than 13 years of experience.
To understand asthma, you need to understand a little about what happens when you breathe.
Normally, with every breath you take, air goes through your nose and down into your throat, into your airways, eventually making it to your lungs. There are lots of small air passages in your lungs that help deliver oxygen from the air into your bloodstream.
Asthma symptoms occur when the lining of your airways swell and the muscles around them tighten. The mucus then fills the airways, further reducing the amount of air that can pass through.
These conditions then bring on an asthma “attack,” the coughing and tightness in your chest that is typical of asthma.
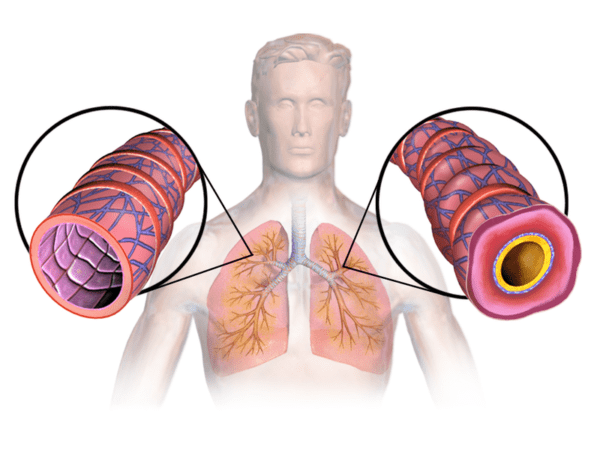
Cause Of Asthma
- Genetics: If a parent has asthma, you’re more likely to develop it.
- History of viral infections: People with a history of viral infections during childhood are more likely to develop the condition.
- Hygiene hypothesis: This hypothesis proposes that babies aren’t exposed to enough bacteria in their early months and years. Therefore, their immune systems don’t become strong enough to fight off asthma and other conditions.
- Early allergen exposure: Frequent contact with possible allergens and irritants may increase your risk of developing asthma.
Risk Of Asthma
- Having a blood relative (such as a parent or sibling) with asthma.
- Having another allergic condition, such as atopic dermatitis or allergic rhinitis (hay fever).
- Being overweight.
- Being a smoker.
- Exposure to secondhand smoke.
- Exposure to exhaust fumes or other types of pollution.
Prevention
- Follow your asthma action plan: Dr. Anand Singh asthma specialist in The Clementine Churchill Hospital in Harrow, and Syon Clinic in Brentford, West London, OSD Healthcare Hertfordshire and the health care team write a detailed plan for taking medications and managing an asthma attack. Then be sure to follow your plan. Asthma is an ongoing condition that needs regular monitoring and treatment. Taking control of your treatment can make you feel more in control of your life in general.
- Get vaccinated for Influenza and Pneumonia: Staying current with vaccinations can prevent flu and pneumonia from triggering asthma flare-ups.
- Identify and avoid Asthma Triggers: A number of outdoor allergens and irritants ranging from pollen and mold to cold air and air pollution — can trigger asthma attacks. Find out what causes or worsens your asthma, and take steps to avoid those triggers.
- Monitor your Breathing: You may learn to recognize warning signs of an impending attack, such as slight coughing, wheezing, or shortness of breath. But because your lung function may decrease before you notice any signs or symptoms, regularly measure and record your peak airflow with a home peak flow meter.
Diagnosis
Physical exam
To rule out other possible conditions — such as a respiratory infection or chronic obstructive pulmonary disease (COPD) – Dr. Anand Singh, will do a physical exam and ask you questions about your signs and symptoms and about any other health problems.
Additional tests
Other tests to diagnose asthma include:
- Imaging tests
- Allergy testing and blood tests
- Sputum eosinophils.
- Provocative testing for exercise and cold-induced asthma.
- Tests to measure lung function
Treatment Of Asthma
Treatments for asthma fall into primary categories: Rescue or first aid treatments and long-term asthma control medications.
Dr. Anand Singh, an Asthma specialist in The Clementine Churchill Hospital in Harrow, Syon Clinic in Brentford West London, OSD Healthcare Hertfordshire will determine the right treatment or combination of treatments for you based on the type of asthma you have, your age, and your triggers.
● ABOUT DR ANAND SINGH
About Dr Anand Singh
Dr Anand Singh is a highly experienced Consultant Respiratory Physician with over a decade of experience in the field.
Dr Singh is a well known Chest Consultant and Sleep Consultant who provides personalised treatment plan.
Dr Anand Singh is a consultant Respiratory Physician at West Hertfordshire Teaching Hospitals NHS Trust
(Watford General and Hemel Hempstead Hospital where he leads the Sleep and Non-Invasive ventilation Service
and Respiratory High Dependency unit. He undertakes sub-speciality clinics in Interstitial Lung diseases
and Sleep Apnoea as well as conducting general respiratory medicine clinics.
Professional Memberships


Recommended by patients
Bronchitis
Bronchitis is an inflammation of the bronchial tubes, the airways that carry air to your lungs. It causes a cough that often brings up mucus. It can also cause shortness of breath, wheezing, a low fever, and chest tightness. Dr. Anand Singh is a bronchitis specialist in The Clementine Churchill Hospital in Harrow, and Syon Clinic in Brentford, West London, OSD Healthcare Hertfordshire treated thousands of patients successfully. Bronchitis treatment consists of self care and cough medications. There are two main types of bronchitis: acute and chronic.
Chronic bronchitis is one type of COPD (Chronic Obstructive Pulmonary Disease). The inflamed bronchial tubes produce a lot of mucus. This leads to coughing and difficult breathing. Cigarette smoking is the most common cause. Breathing in air pollution, fumes, or dust over a long period of time may also cause it.
To diagnose chronic bronchitis treatment, your doctor will look at your signs and symptoms and listen to your breathing. You may also have to undergo other tests.
Cause of Bronchitis
Most often, the same viruses that give you a cold or the flu cause acute bronchitis. But sometimes, bacteria bring it on.
In both of these cases, as your body fights the germs, your bronchial tubes swell and make more mucus. That means you have smaller openings for air to flow through, which can make it harder to breathe.
Chronic bronchitis causes include:
- Breathing in air pollution and other things that bother your lungs, like chemical fumes or dust, over time.
- Smoking or breathing in secondhand smoke for a long time.
Risk
Dr. Anand Singh – Bronchitis specialist in The Clementine Churchill Hospital in Harrow, and Syon Clinic in Brentford, West London, OSD Healthcare Hertfordshire believes that you have a bigger chance of getting either kind of bronchitis if:
- You smoke.
- You have asthma and allergies.
- You have a weaker immune system.
Prevention
To lower your chances of getting acute bronchitis or a flare-up of chronic bronchitis Dr. Anand Singh gives these 5 important precautions:
- Stay away from cigarette smoke.
- Get the flu vaccine since you can get bronchitis from the flu virus.
- Make sure your pertussis vaccine is up to date.
- Wash your hands often.
- Wear a mask when you’re around things that bother your lungs, such as paint fumes.
Diagnosis
Your doctor usually can tell whether you have bronchitis based on a physical exam and your symptoms. They’ll ask about your cough, such as how long you’ve had it and what kind of mucus comes up with it. They’ll also listen to your lungs to see whether anything sounds wrong, like wheezing.
Your doctor may need to do some tests like
- Check the oxygen levels in your blood.
- Do a lung function test.
- Give you a chest X-ray.
- Order blood tests.
- Test your sputum /mucus to rule out diseases caused by bacteria.
Treatment of Bronchitis
Most of the time, acute bronchitis goes away on its own within a couple of weeks.
If yours is caused by bacteria (which is rare), your doctor may give you antibiotics. If you have asthma or allergies, or you’re wheezing, they might suggest an inhaler. This helps open your airways and makes it easier to breathe.
To ease your acute bronchitis symptoms, you can:
- Drink a lot of water
- Get plenty of rest
- Use a humidifier or steam
● ABOUT DR ANAND SINGH
About Dr Anand Singh
Dr Anand Singh is a highly experienced Consultant Respiratory Physician with over a decade of experience in the field.
Dr Singh is a well known Chest Consultant and Sleep Consultant who provides personalised treatment plan.
Dr Anand Singh is a consultant Respiratory Physician at West Hertfordshire Teaching Hospitals NHS Trust
(Watford General and Hemel Hempstead Hospital where he leads the Sleep and Non-Invasive ventilation Service
and Respiratory High Dependency unit. He undertakes sub-speciality clinics in Interstitial Lung diseases
and Sleep Apnoea as well as conducting general respiratory medicine clinics.
Professional Memberships


Recommended by patients
Chronic Obstructive Pulmonary Disease
Chronic Obstructive Pulmonary Disease (COPD) is a preventable and treatable lung disease. People with COPD must work harder to breathe, which can lead to shortness of breath and/or feeling tired. Early in the disease, people with COPD may feel short of breath when they exercise. As the disease progresses, it can be hard to breathe out (exhale) or even breathe in (inhale).
A person with COPD may have Chronic bronchitis , emphysema, or a combination of both conditions. The amount of each of these conditions differs from person to person.
Asthma is another disease that causes narrowing of the airways, making it hard to breathe at times, but asthma is not included in the definition of COPD. Some people do have a mix of both COPD and asthma.

What is Chronic Bronchitis?
This involves inflammation of the lining of the bronchial tubes that carry air to and from your lungs. The condition develops over time and is characterised by a long-lasting cough and mucus production.
What is emphysema?
The lungs are made up of more than 300 million tiny air sacs called alveoli. These air sacs are normally stretchy and springy. When you breathe in, the air sacs expand like tiny balloons. Breathing out is usually passive (takes no effort) as the alveoli “spring” back to their original size. In emphysema, the walls of the air sacs (alveoli) of the lung are damaged and lose their stretchiness. As a result, they do not empty easily. Emphysema can also contribute to the narrowing of the airways.
The combination of non-stretchy alveoli due to emphysema and narrowed airways due to both Chronic bronchitis and emphysema prevents the lungs from emptying normally. This causes air to become trapped in the lungs. “Air trapping” or the inability to fully exhale, leads to abnormal expansion or hyperinflation of the lungs. Constantly having trapped air in the lungs combined with the extra effort needed to breathe results in a person feeling short of breath.
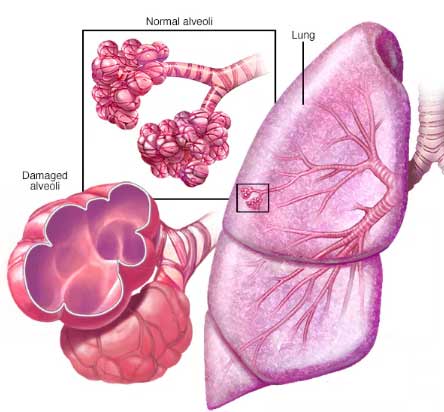
What causes COPD?
Although the most common cause of COPD is tobacco smoke, there are several other factors that can cause or make COPD worse, including environmental exposures and genetic (inherited) risk. For example, heavy exposure to certain dust at work, chemicals, and indoor or outdoor air pollution (including wood smoke or biomass fuels) can contribute to COPD.
How do I know if I have COPD?
Common signs and symptoms of COPD:
- Shortness of breath, also called “dyspnea,” while doing everyday activities
- Constant coughing or wheezing sometimes called a “smoker’s cough”
- Chest tightness or inability to take a deep breath
- Recurring respiratory infections
Loss of energy - A blue hue around the lips and fingernail beds called “cyanosis”
- Unintended weight loss
If you have these symptoms, you should talk to your healthcare provider. Some people with early COPD may not be aware of symptoms.
Testing should be done in people who are at risk for COPD. Your healthcare provider may have you do a breathing test (lung function test) called spirometry. Spirometry measures your ability to exhale and can detect whether your airways are narrowed.
How does a healthcare provider know a person has COPD?
Healthcare providers diagnose COPD based upon the combination of symptoms and test results. The single most important test to determine if a person has COPD is Lung function testing . Changes of COPD can also be seen on a chest x-ray or a chest CT scan. Once your healthcare provider has determined that you have COPD, he may order other tests to assess how well you are breathing with sleep and with exercise (six-minute walk test). This includes looking at your oxygen saturation levels .
How is COPD treated?
- The first and most important treatment of COPD in smokers is to stop smoking. Medications and other therapies are available to help treat nicotine addiction and to help you stop smoking.
- Medications can also be prescribed to help relieve symptoms of COPD and to prevent symptom flares (called exacerbations) that can lead to further loss of lung function. Some general classes of medications include those that aim to widen the airways (bronchodilators), reduce swelling in the airways (anti-inflammatory drugs, such as steroids), and/or treat infections (antibiotics). Other than antibiotics, most COPD medications should be taken every day, usually for life.
- Avoid contact with those who are sick, wash hands often, get a yearly flu vaccine, and get a pneumonia vaccine when recommended by your healthcare provider.
- In some people, COPD can also cause the oxygen level in the blood to be low. If this occurs, a person can be given supplemental oxygen if there is no active smoker at home .
- Proper nutrition and staying in good physical shape are also important, not just for symptom relief but also for your quality of life.
- Pulmonary rehabilitation programs offer supervised exercise and education for those with breathing problems and should be a part of a comprehensive treatment plan for anyone with COPD.
- In some cases, surgical procedures such as lung volume reduction surgery or lung transplantation may be options to consider.
- If you have COPD, it’s important to make sure that other diseases you may have, such as high blood pressure, heart disease, diabetes, and asthma, also are being treated.
Will COPD ever go away?
The term chronic, in chronic obstructive pulmonary disease, means that it lasts for a long time. Symptoms of COPD sometimes improve when a person stops smoking, takes medication regularly, and/or attends pulmonary rehabilitation.
However, the lungs are still damaged and can never fully return to normal. Therefore, COPD is a lifelong condition. Breathlessness and fatigue may never go away entirely, but people can learn to manage their condition and continue to lead a fulfilling life.
● ABOUT DR ANAND SINGH
About Dr Anand Singh
Dr Anand Singh is a highly experienced Consultant Respiratory Physician with over a decade of experience in the field.
Dr Singh is a well known Chest Consultant and Sleep Consultant who provides personalised treatment plan.
Dr Anand Singh is a consultant Respiratory Physician at West Hertfordshire Teaching Hospitals NHS Trust
(Watford General and Hemel Hempstead Hospital where he leads the Sleep and Non-Invasive ventilation Service
and Respiratory High Dependency unit. He undertakes sub-speciality clinics in Interstitial Lung diseases
and Sleep Apnoea as well as conducting general respiratory medicine clinics.
Professional Memberships


Recommended by patients
What is Tuberculosis (TB)?
Tuberculosis is a contagious disease that is transmitted from person to person through coughing and breathing in airborne droplets that contain bacteria. TB primarily affects the lungs
but can affect any part of the body. Dr. Anand Singh is a TB specialist inThe Clementine Churchill Hospital in Harrow, and Syon Clinic in Brentford, West London, OSD Healthcare Hertfordshire and has vast experience in managing tuberculosis cases.
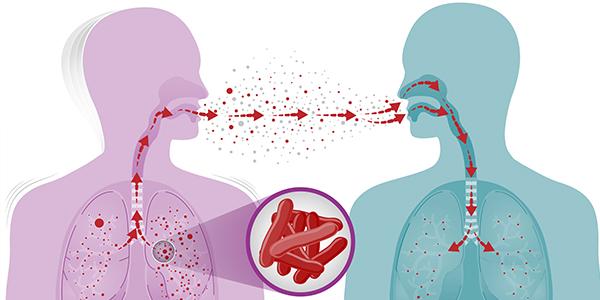
What causes TB?
TB is caused by slow-growing bacteria called mycobacterium tuberculosis. When these bacteria enter the lungs, they are usually walled off into harmless capsules (granulomas)
in the lung, causing the infection but not a disease. These capsules may later wake up weeks, months, or decades later causing active TB disease.
Who gets TB infection and TB disease?
People who are more likely to acquire TB infection are the following:
- People recently exposed to someone who has symptomatic TB disease.
- People who live in congregate settings with high-risk persons.
- People who live or have lived in countries where TB is common; or
- People who are health care workers who are in contact with TB patients when proper infection control procedures are not followed.
Many people who acquire TB infection do not have symptoms and may never develop TB disease. These people have latent TB infections (LTBI). However, people with TB infection who have weaker immune systems due to diabetes, HIV infection, kidney failure, or take
certain immunosuppressive medications such as TNF-alpha blockers may be more likely to develop active TB disease with symptoms.
What are the signs and symptoms of TB disease?
Symptoms are usually mild and tend to present over a period of weeks, months. TB disease symptoms are often initially mistaken for a smoker’s cough, allergies, or chronic bronchitis from a lingering cold or flu infection. TB infection most often affects the lungs but can cause problems in other parts of the body. The classic symptoms of TB in the lungs include:
- Cough lasting more than two weeks
- Unexplained weight loss
- Low-grade fever
- Night sweats
How is TB diagnosed?
TB disease is often diagnosed by microscopic examination of ideally 3 separate samples of sputum (phlegm) often collected on different days. The sputum is first looked at under a microscope using a special dye (acid-fast bacillus AFB stain) to see if any TB bacteria can be found. It is not always positive as there may be only a small number of bacteria so the culture is always needed. Sputum cultures are done to grow the bacteria to confirm the diagnosis and determine the best combination of drugs for treatment. Sputum for genetic testing for TB bacilli ( Tb Pcr / Gene expert) gives a better yield. Dr. Anand Singh– a TB specialist in The Clementine Churchill Hospital in Harrow, and Syon Clinic in Brentford, West London, OSD Healthcare Hertfordshire would occasionally do a Bronchoscopy to obtain lung samples if a patient is unable to produce sputum. In addition to these tests, chest X-rays and CT chest imaging are performed to evaluate for any lung abnormalities. If TB is suspected in a different part of the body, a different sample or a tissue biopsy may be needed.
How is TB treated?
Tuberculosis disease is usually treated with 4 anti-TB medications for at least six months. If TB is in the bones, brain, or other hard-to-reach areas, treatment will be longer. This can mean taking 6-12 pills per day! Many patients find this difficult without the support of workers trained in providing directly observed treatment (DOT).
Drug-Resistant TB requires Longer treatment from 12 months to 2 ½ years.
How can I prevent TB?
TB is spread by tiny airborne droplets created by coughing. Dr. Anand Singh -TB specialist in The Clementine Churchill Hospital in Harrow, and Syon Clinic in Brentford, West London, OSD Healthcare Hertfordshire is of the opinion that Covering the mouth and nose when coughing is an important way to stop the spread of TB and other airborne diseases. If you have TB disease and are coughing, it is important to wear a mask and limit contact with others until your health care provider tells you that you are no longer. contagious while on treatment. Seeking care right away and finding out you have TB is the best way to stop its spread since the treatment of the disease helps you not be contagious, decreasing transmission.
Common side effects of anti TB drugs and it’s treatment
- Do not take all the medicines together.
- Do not keep yourself hungry.
- Do not keep a gap of more than 2-3 hours between two meals.
- Avoid smoking and alcohol consumption as it aggravates acidity.
- Inform your treatment supporter, health worker, or doctor without any delay.
Burning Sensation In Lower Part Of Chest & Pain In Upper Abdomen
Rashes With Or Without Itching on Hands Or Legs
- Apply moisturizing cream
- Do not expose the rashes to sunlight.
- Rashes usually subside with time
- Inform your treatment supporter, health worker or doctor without any delay
Nausea & Vomiting, Loose Stools / Diarrhoea
- Do not take all the medicines together.
- Take medicines with little water or milk at bedtime.
- Stay hydrated (drink enough water)
- Avoid smoking and alcohol consumption as it aggravates these sufferings.
- Inform your treatment supporter, health worker, or doctor without any delay.
- Do not take any medicines on your own. Do not stop or reduce the dose of anti-TB medicines on your own.
Headache, Giddiness & Weakness
- Have nutritious food and enough water.
- Take proper rest.
- Follow a healthy lifestyle (yoga, meditation, etc.).
- Stay positive.
- Inform your treatment supporter, health worker, or doctor without any delay.
● ABOUT DR ANAND SINGH
About Dr Anand Singh
Dr Anand Singh is a highly experienced Consultant Respiratory Physician with over a decade of experience in the field.
Dr Singh is a well known Chest Consultant and Sleep Consultant who provides personalised treatment plan.
Dr Anand Singh is a consultant Respiratory Physician at West Hertfordshire Teaching Hospitals NHS Trust
(Watford General and Hemel Hempstead Hospital where he leads the Sleep and Non-Invasive ventilation Service
and Respiratory High Dependency unit. He undertakes sub-speciality clinics in Interstitial Lung diseases
and Sleep Apnoea as well as conducting general respiratory medicine clinics.
Professional Memberships


Recommended by patients